Summary by James R. Martin, Ph.D., CMA
Professor Emeritus, University of South Florida
ABC Main Page | Time-driven ABC Bibliography
| Health Care Cost Main Page
This article provides the text of an interview with Kaplan and Porter conducted by Mark Frigo. The problem discussed is how to manage the true costs and value of health care.
The first question Frigo asked is how Kaplan and Porter got together to address the health care issue. Porter mentions his earlier work and the Value-Based Health Care Agenda described in a 2013 article by Porter and Lee (See the related summaries below). Porter called Kaplan in 2010 explaining that health care needed a better way to measure cost. Kaplan responded that time-driven activity-based costing would work well in health care, but he had not found a hospital willing to give it a chance. Porter had connections with some hospitals that were open to implementing a new cost system, and the Kaplan-Porter partnership to build a proper foundation for value-based health care began.
Frigo's second question: "What are the most important contributions management accountants can make in this area?" Kaplan's response is that management accountants can play a critical role in providing more valid measurements of cost and outcomes and in designing value-based payment models like bundled payments that cover the treatment of a patient's medical condition.
The third question is related to what tools and approaches are used in the value-based agenda to help health care organizations create greater value. Porter responds that value improvement means better outcomes for patients relative to the costs of achieving those outcomes. The most powerful step is to start measuring outcomes at the patient level for a given medical condition, including the functional status of patients after treatment. A sufficient set of outcomes should be developed and standardized for every major medical condition. The International Consortium for Health Outcomes Measurement has currently published 20 sets of outcomes covering 45% of the disease burden in the U.S.
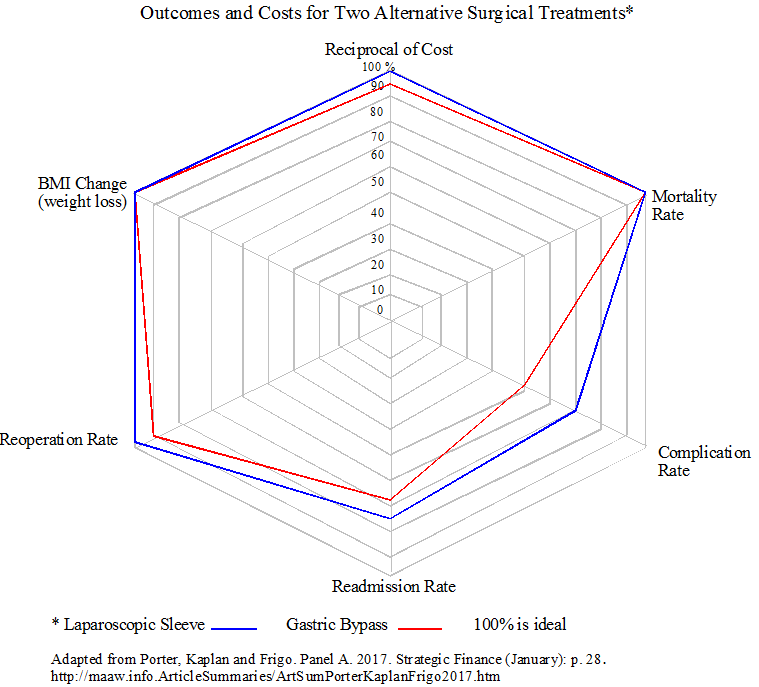
The article includes four radar charts that illustrate the value-based framework. I developed two adaptations to show how both outcomes and cost can be presented in a visual way to compare procedures and surgeons. The first chart below, based on data from Scottsdale Healthcare, compares two alternative surgical treatments for obesity. The scale is from 0-100% where 100% is ideal. Cost is plotted as the reciprocal of the cost based on time-driven ABC. It is fairly easy to see from the illustration that sleeve surgery provides better outcomes and cost compared to gastric bypass. Sleeve surgery cost less than gastric bypass, and also involves fewer complications, readmissions, and reoperations.

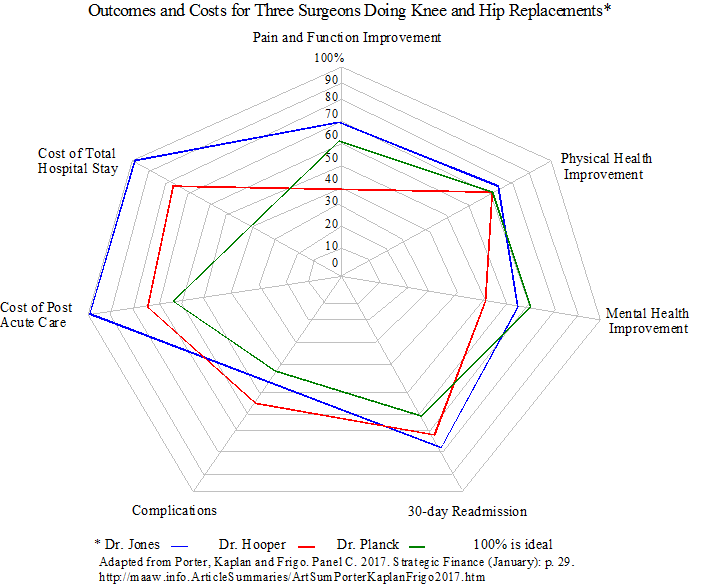
The second illustration compares outcomes and costs for three surgeons who perform total knee and hip replacements. Physical health improvement and mental health improvement are measured by KOOs Jr. PROMIS-10 and other measurement tools. Dr. Jones has lower costs in terms of both cost of post acute care and total hospital stay, somewhat better physical health improvement, fewer 30-day readmissions, and fewer complications than the other two surgeons. Sharing best practices is the most powerful way to improve health care outcomes and costs across health care systems.
Question four is essentially, What is wrong with current health care cost systems? Kaplan says that health care cost have been based on charges and only for reimbursed services leaving the cost of non-reimbursed services buried in arbitrary allocated overhead cost pools. Administrators tend to apply arbitrary cuts at the line-item level, or across-the-board cuts in personnel costs. However, sustainable cost reduction requires knowledge of the structure of health care delivery. This means understanding how money is spent to treat patients for specific medical conditions.
Question five: How is time-driven activity-based costing being used in the Value-based Health Care Delivery initiative? Time-driven ABC is a bottom up approach where clinical and administrative processes are mapped and capacity cost rates are estimated for personnel and equipment. Team members start by identifying the events in the care cycle including which personnel and equipment resources are used at each activity, and the number of minutes each resource is used. Dollar per minute capacity rates are developed for each clinical resource based on the capacity measured in hours or minutes that each resource is available for productive work. These rates are multiplied by the time each resource spends in the process. The total cost of caring for the patient is the sum of all the process steps over the entire care cycle. See the Kaplan and Porter 2011 summary below for an example.
Kaplan states that they have conducted several multisite studies that show very large cost differences between providers. Using variance analysis they are able to isolate the cost differences due to prices paid for personnel and other resources, and the cost differences due to provider inefficiency. This helps identify the best practices that can then be used to reduce the costs of inefficient providers without harming patients.
Question six: Can you describe an example or two of the pilot studies you have been involved with? One example Kaplan mentioned involved the cost savings discovered when comparing joint replacement patients who received rehabilitation at home (about $1,000), versus rehabilitation at a nursing facility (about $6,000). Another example revealed savings when surgeons could schedule two operating rooms, as opposed to just one. Administrators wanted to fully utilize their operating rooms, but the study showed that a fully equipped operating room cost about $.50 per minute, while a surgical team cost more than $20 per minute. Clearly, the surgical team is the resource that needs to be fully utilized.
Question seven to Porter and Kaplan: "What do you hope will be the future positive outcomes from your work? Their response is that they hope to have generally accepted standard outcome measurement sets for 90% of the medical conditions represented by the world's disease burden. They also hope providers will embrace the idea of mapping processes for all their care cycles at the medical condition level, and that bundled payments (a single payment covering all the care for a patient's medical condition and treatment over a specific time frame) will become the dominant payment mechanism. This will lower costs and simultaneously provide patients with better outcomes.
____________________________________________
Related Time-driven ABC summaries:
Kaplan, R. S. and M. E. Porter. 2011. How to solve the cost crisis in health care: The biggest problem with health care isn't with insurance or politics. It's that we're measuring the wrong things the wrong way. Harvard Business Review (September): 46-64. (Time-driven ABC applied to health care). (Summary).
Kaplan, R. S. and S. R. Anderson. 2007. The innovation of time-driven activity-based costing. Cost Management (March/April): 5-15. (Summary).
Kaplan, R. S. and S. R. Anderson. 2004. Time-driven activity-based costing. Harvard Business Review (November): 131-138. (Summary).
Porter, M. E. and T. H. Lee. 2013. The strategy that will fix health care: Providers must lead the way in making value the overarching goal. Harvard Business Review (October): 50-67. (This article shows how the time-driven ABC approach fits into the strategic value agenda for a high-value health care delivery system). (Summary).
Other Related summaries:
Anderson, S. W., J. W. Hesford and S. M. Young. 2002. Factors influencing the performance of activity based costing teams: A field study of ABC model development time in the automobile industry. Accounting, Organizations and Society 27(3): 195-211. (Summary).
Bast, J. L., R. C. Rue and S. A. Wesbury Jr. 1993. Why we spend too much on Health Care and what we can do about it. Heartland Institute. (Summary).
Brausch, J. M. and T. C. Taylor. 1997. Who is accounting for the cost of capacity? Management Accounting (February): 44-46, 48-50. (Summary).
Church, A. H. 1995. Overhead: The cost of production preparedness. Journal of Cost Management (Summer): 66-71. (Reprint of Church, A. H. 1931. Overhead: The cost of production preparedness. Factory and Industrial Management (January): 38-41. (Summary).
Cooper, R. 1990. Implementing an activity-based cost system. Journal of Cost Management (Spring): 33-42. (Summary).
Cooper, R. and R. S. Kaplan. 1992. Activity-based systems: Measuring the costs of resource usage. Accounting Horizons (September): 1-13. (Summary).
Cooper, R., and R. S. Kaplan. 1998. The promise - and peril - of integrated cost systems. Harvard Business Review (July-August): 109-119. (Summary 1, (Summary 2).
Debruine, M. and P. R. Sopariwala. 1994. The use of practical capacity for better management decisions. Journal of Cost Management (Spring): 25-31. (Summary).
Gantt, H. L. 1994. The relation between production and costs. Journal of Cost Management (Spring): 4-11. This is a presentation Gantt made in 1915. (Summary).
Kaplan, R. S. 1990. The four stage model of cost systems design. Management Accounting (February): 22-26. (Summary).
Krumwiede, K. R. 1998. ABC: Why it's tried and how it succeeds. Management Accounting (April): 32-34, 36, 38. (Summary).
Mangan, T. N. 1995. Integrating an activity-based cost system. Journal of Cost Management (Winter): 5-13. (Summary).
Martin, J. R. 2000. The advantages of teaching three production volume variances. Journal of Accounting Education 18(1): 35-50. (ABC variance analysis based on an example from Kaplan, R. S. and R. Cooper. 1998. Cost and Effect: Using Integrated Cost Systems to Drive Profitability and Performance. Boston: Harvard Business School Press).
Martin, J. R. Not dated. Chapter 7: Activity Based Product Costing. Management Accounting: Concepts, Techniques & Controversial Issues. Management And Accounting Web. Chapter7.htm
McNair, C. J. 1994. The hidden costs of capacity. Journal of Cost Management (Spring): 12-24. (Summary).
Mecimore, C. D. and A. T. Bell. 1995. Are we ready for fourth-generation ABC? Management Accounting (January): 22-26. (Summary).