Summary by James R. Martin, Ph.D., CMA
Professor Emeritus, University of South Florida
Health Care Cost Main Page | Time-driven ABC Bibliography
Health care systems around the world are facing rising costs and uneven quality. The purpose of this article is to describe a new broad strategy for achieving the best patient outcomes at the lowest cost. Porter and Lee refer to the new strategy as the value agenda that includes transforming how health care delivery is organized, measured, and reimbursed.
Defining the Goal
The first step is to define the goal as improving value for patients. This means improving health outcomes that matter to patients relative to the cost of achieving those outcomes, rather than simply increasing volumes and maintaining margins. The current health care system is based on independent private practice physicians, measurements of quality based on compliance, cost accounting driven by charges rather than outcomes, fee-for-service payments by specialty, delivery with duplicate service lines, fragmented patient populations, and siloed IT systems. With these old systems in place, providers are facing a changing environment where reimbursement rates from Medicare and Medicaid do not cover the provider's cost, and their fee-for-service revenue approach is under pressure from competition by national retailers who are offering in-store clinics. In addition, employers and insurers are reducing benefits and raising deductibles. Facing lower payment rates and loss of market share, providers obviously need a new strategy.
The Strategy for Value Transformation
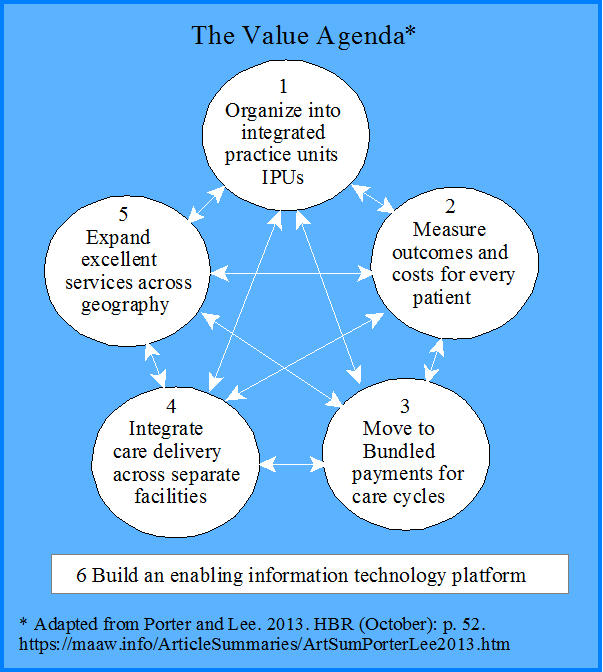
The new strategic agenda has six interdependent and mutually reinforcing components:
1. Organize into Integrated Practice Units (IPUs)
Organizing into integrated practice units means organizing by the patient's medical condition rather than by siloed specialty departments. IPUs treat the problems and complications associated with a specific medical condition, as well as provide the education, counseling and support for needed behavioral changes to maximize the patients overall outcome. IPU members are either co-located, or closely connected if based in different locations, to facilitate communication, collaboration, and efficiency, and to avoid the typical duplication of effort, delays and inefficiency associated with the current system. The IPU multidisciplinary team is responsible for the full cycle of care, patient education, follow-up, measuring the outcomes, costs and processes for each patient, and with joint accountability for outcomes and costs.
2. Measure Outcomes and Costs for Every Patient
Perhaps the most important step is measuring the value of health care for patients. This means measuring outcomes and costs, and the only true measure of quality are the outcomes that matter to patients. There are three tiers of measures that matter to patients for a specific medical condition. One involves the health status achieved. A second tier is related to the cycle of care and recovery including the patients discomfort, and unnecessary anxiety caused by delays, chaos, confusion and unnecessary setbacks. A third tier involves the sustainability of health. Measuring the outcomes that matter to patients provides a powerful tool for cost reduction by providing a way for health care providers globally to make comparisons that stimulate improvement.
Current systems for measuring the cost of health care are department-based and designed around fee-for-service contracts. However, providers must measure the cost at the patient level for a medical condition over the full cycle of care. Time-driven activity-based costing provides a way do this. See the summary of Kaplan and Porter's 2011 paper below for the steps involved in the time-driven ABC cost measurement process.
3. Move to Bundled Payments for Care Cycles
The dominant payment models in health care include global capitation and fee-for-service. Global capitation provides a single payment to cover all of a patient's needs, but not for improving outcomes or value. The fee-for-service model motivates providers to increase volume, but not value. Bundled payments covers the full cycle of care and encourages high value health care at the patient level.

4. Integrate Care Delivery Systems
The majority of health care systems are multisite organizations with loose confederations of stand-alone units that often duplicate services. There are four components needed to achieve the integration that would eliminate the fragmentation and duplication. The first is to define the scope of services recognizing that every facility can't do everything for everyone. Value-based health care delivery requires limiting the range of services that are offered. The second component involves concentrating volume in fewer locations so that providers gain the experience needed to improve outcomes and reduce costs. The third component is to choose the right location for each service where the skills needed are matched with the complexity of the service. This will increase staff productivity, reduce cost and avoid situations where high fees are charged for routine services performed in high cost settings. The final component is to integrate health care for individual patients across locations.
5. Expand Geographic Reach
Geographic expansion can take the form of the hub-and-spoke model, or the clinical affiliation model, but the key is that superior providers need to serve more patients. In the hub-and-spoke model patients receive their initial evaluation at the hub, but most of the care takes place in more-convenient locations. In the clinical affiliation model the integrated practice unit (IPU) uses a community provider's local facilities rather than adding capacity. The IPU provides some staff as well as oversight for clinical care.
6. Build an Enabling Information Technology Platform
The value-enhancing IT platform includes six elements:
It is centered on patients and follows them across services, sites and the full cycle of care.
It uses common data definitions and data fields for diagnoses, lab values, treatments and the other aspects of care.
It includes all types of patient data such as physician notes, images, chemotherapy orders, lab tests and other related data.
All parties involved in the patient's health care have access to the medical records.
Templates and expert systems for each medical condition are included in the system.
The system architecture is designed to make it easy to extract information.
Getting Started
Implementing the value agenda takes an open-ended commitment starting with defining the goal as improving value for patients. It is a journey that requires strong leadership. Organizations that adopt the value agenda will reap huge benefits including financial viability and a reputation of excellence in outcomes and value. Providers that cling to today's broken health care system will find it more difficult to maintain market share and will eventually become dinosaurs.
_________________________________________
Summaries related to Time-driven ABC:
Kaplan, R. S. and M. E. Porter. 2011. How to solve the cost crisis in health care: The biggest problem with health care isn't with insurance or politics. It's that we're measuring the wrong things the wrong way. Harvard Business Review (September): 46-64. (Time-driven ABC applied to health care). (Summary).
Kaplan, R. S. and S. R. Anderson. 2007. The innovation of time-driven activity-based costing. Cost Management (March/April): 5-15. (Summary).
Kaplan, R. S. and S. R. Anderson. 2004. Time-driven activity-based costing. Harvard Business Review (November): 131-138. (Summary).
Kaplan, R. S., M. E. Porter and M. L. Frigo. 2017. Managing healthcare costs and value. Strategic Finance (January): 24-33. (Summary).
Other related summaries:
Bast, J. L., R. C. Rue and S. A. Wesbury Jr. 1993. Why we spend too much on Health Care and what we can do about it. Heartland Institute. (Summary).
Caltrider, J., D. Pattison and P. Richardson. 1995. Can cost control and quality care coexist? Management Accounting (August): 38-42. (Summary).
Cohen, F. 2011. Improving processes in your practice: Do the same thing with less, or more with the same thing with lean six sigma and lean principles in your toolbox. Medical Economics (June): 60-62,-67-69. (Note).
Davenport, T. H. and J. Glaser. 2002. Just-in-time delivery comes to knowledge management. Harvard Business Review (July): 107-111. (Summary).
De Luca, M. 2018. How lean accounting promotes lean in the organization. Cost Management (January/February): 21-26. (Summary).
Esquire. 2015. America: These are your choices. Esquire (December/January): 149-153, 160-161, 164, 168. (Summary - Summary of ten questions related to the most critical choices for America based on information from the Brookings Institution. One of the questions is related to Obamacare).
Kershaw, R. 2000. Using TOC to ‘cure’ healthcare problems. Management Accounting Quarterly (Spring): 22-28. (Summary).
Porter, M. E. 1980. Competitive Strategy: Techniques for Analyzing Industries and Competitors. The Free Press. (Summary).
Porter, M. E. 1996. What is a strategy? Harvard Business Review (November-December): 61-78. (Summary).
West, T. D. and D. A. West. 1997. Applying ABC to healthcare. Management Accounting (February): 22, 24-26, 28-30, 32-33. (Summary).